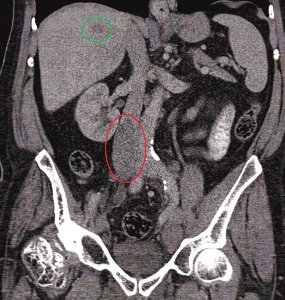
An unusual case of bowel perforation in a 9 month old infant
In Australia, between 2009 and 2010 almost 290 000 cases of suspected child abuse and neglect were reported to Australian state and territory authorities. Child maltreatment may present insidiously, not …