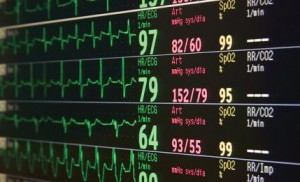
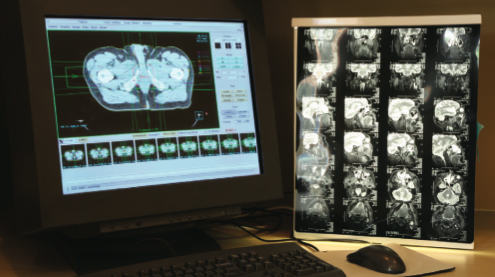
Recognition and response to the clinically deteriorating patient
Background: Early recognition of clinical deterioration has been associated with a lower level of intervention and reduced adverse events. A widely-used approach in Australia is the Medical Emergency Team (MET) …