Sixth Year Medicine (Undergraduate)
University of Western Australia
Tarryn Sohn
Fourth Year Medicine (Undergraduate)
University of Western Australia
Tarryn is a fourth year medical student at the University of Western Australia.
Wednesday, April 30th, 2014
This paper is the first to document the mechanism of how a mobile segment of the hook of hamate can dynamically compress the motor branch of the ulnar nerve. Presented is the case of a professional golfer who experienced pain on the ulnar aspect of his right hand that he attributed to weakness and inability to control his hand. Imaging revealed the rare condition of os hamulus proprius causing a dynamic compression of the ulnar nerve when in power grip. Provided is a review of wrist anatomy with particular focus on the peculiar case of the bipartite hamulus.
Introduction
Anatomy of the wrist
The wrist comprises a proximal and distal carpal row. The distal carpal row consists of the trapezium, trapezoid, capitate and hamate and acts as a base for the metacarpals. The proximal carpal row consists of the scaphoid, lunate, triquetrum and pisiform bone. These function as an intercalated segment, balancing the hand on the radius and ulna. [13]
Hamate anatomy and function
The hamate articulates with the triquetrum proximally and the bases of the 4th and 5th finger metacarpals distally. The hook of the hamate is an important structure in the hand. Protruding from the volar surface of the hamate, it anchors the distal transverse carpal ligament, acting as a pulley for the ulnar flexor tendons and protecting the motor branch of the ulnar nerve. This branch of the ulnar nerve courses dorsally and distally around the hook of the hamate to supply nearly all the intrinsic muscles of the hand. [14]
Guyons Canal and the Ulnar Nerve
Felix Guyon described a potential space [15], which is a fibro-osseous tunnel, protecting the ulnar nerve and artery and veins as they enter the hand. The boundaries of Guyon’s canal are the pisiform bone, the tip of the hook of the hamate, the piso-hamate ligament and the transverse carpal ligament.
Os Hamulus proprium
The os hamulus ossifies from a primary ossification center in the body of the hamate; however, occasionally a secondary ossification center in the hook of the hamate is also present. [1] Rarely, the secondary ossification center in the hook of the hamate does not unite with the primary ossification center in the body of the hamate. [2] When the tip of the hook of the hamate does not fuse with the body of the hamate the result is a separate ossicle known as the os hamulus proprium or a bipartite hamulus. Whilst an os hamulus proprium or bipartite hamulus is often congenital a similar appearance can sometimes be the result of a non-union of a fracture of the hook of the hamate. [3]
Ossification of the hamate is not complete until the early teenage years. [4] Bone growth and maturation usually takes place via a single ossification center. However, a secondary ossification center independent from associated underling bone occasionally develops giving rise to an accessory ossicle. [9] This lack of fusion has been observed involving the hamulus and the hamate and is known as either os hamulus proprium or bipartite hamulus. Such cases are often congenital in nature; however, depending on the patient’s history, trauma or degenerative etiology should be considered. [10]
A study [5] conducted in 2005 on 3,218 hand radiographs revealed that variations are more prevalent than previously thought. 96 participants were found to have variations of the hook of hamate of which 42 patients had a bipartite hook, 50 had a hypoplastic hook and 4 had an aplastic hook. Furthermore, 93 of these cases presented with carpal tunnel syndrome symptoms.
In 1981, Greene et al. [6] identified a single case of bipartite hamulus with ulnar tunnel syndrome. However, since then there have been no other accounts of the os hamulus proprius, associated with dynamic ulnar neuropathy.
Case Study
History
The patient was a 37 year old professional right handed golfer with an unremarkable medical record.
He presented with an eight-week history of pain in the ulnar side of the right hand with loss of fine motor control requiring the use of his contralateral left hand to perform activities of daily living. The patient reported no other neurological symptoms at the time.
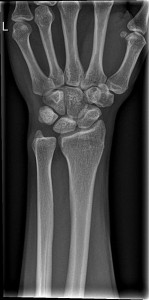
Physical examination revealed wasting of the intrinsic muscles of the right hand, most pronounced in the first dorsal interosseous muscles with weak intrinsic movements when comparison to the left side. Following initial examination a series of investigation and imaging was conducted:
It is not uncommon for golfers to fracture the hook of hamate based on the type of grip and dynamics of the golf swing. Furthermore, they can develop stress fractures of the hook of the hamate, which subsequently do not unite. [11,12]
Whilst this may have been the mechanism for the development of injury, an alternative explanation implicates a congenital anomaly where the primary ossification center the hamate fails to unite with the hook of the hamate giving rise to a bipartite bone (os hamulus proprius). [3]
Findings
This patient had a well-established long-standing asymptomatic non-union of the hamate or an os hamuli proprius, which subsequently became symptomatic following a motor vehicle accident in January 2005 resulting in an acute eight-week history of fine motor control deficit in the right hand.
Surgical intervention
A mobile segment of the hook of the hamate was identified. Pressure over the mobile segment of the hook of the hamate compressed the motor branch of the median nerve as it traversed around the ulnar and distal hook of the hook of the hamate. The motor branch of the median nerve was swollen proximal to the point where the mobile segment of the hook of the hamate dynamically impacted on the nerve. This had the appearance of a ‘neuroma in continuity’ commonly seen from failure of regenerating nerve growth cone to reach peripheral targets.
The ulnar nerve was released in Guyon’s Canal. The motor branch of the ulnar nerve was identified and dissected as it coursed around the hook of the hamate. The hook of the hamate was very mobile and unstable. Manipulation of the mobile hook of the hamate demonstrated how it impacted and compressed the motor branch of the median nerve distal to the swollen segment of the motor branch of the median nerve. This was surgically excised.
The patient noticed a marked improvement of symptoms within two days post-operatively commenting on a return of ‘power and movement’. Following rehabilitation through daily grip strength exercises; this was further demonstrated on clinical examination at eighteen days confirming a return of intrinsic muscle power in the right hand.
The following five images describe the surgical repair of Os Hamulus Proprius as performed in this case.
Discussion
The hook of the hamate is an important structure providing mechanical stability on the ulnar aspect and protecting the motor branch of the ulnar nerve as it traverses deep into the hand from Guyon’s canal. It is also an important structure for insertion of the flexor retinaculum and as a result the muscles on the ulnar side of the hand. [16]
It is very likely that this abnormality of the hook of the hamate was present prior to his injury. The most likely explanation is that it is a secondary ossification center of the hook of the hamate (os hamulus proprius) which went on to unite. However, it is not possible to completely rule out that this represents a long standing non-union of the hook of the hamate and at some stage in the past he may have sustained a stress fracture which resulted in a non-union. [1,3,6,8,11,17]
Clinical examination plays a crucial role in isolating cases of os hamulus proprius. Patients will often present with clinical signs suggesting ulnar neuropathy such as intrinsic muscle weakness and altered sensation of the hand. In differentiating a case of bipartite hamulus, there will also be marked local tenderness over the hook of hamate with symptomatic pain due to dynamic compression such as when performing a power grip. Further hand and upper limb evaluation can compliment the diagnosis by quantifying and comparing loss of strength in the hand. [17]
The patient had marked motor (intrinsic hand muscles) weakness and some minor impairment of sensation in the ulnar distribution, which is consistent with the electrophysiological abnormalities in the hand. Surgery to remove the mobile segment of hamulus resulted in major improvement – particularly in terms of the level of his symptoms and restoration of normal power to the intrinsic muscles of the hand. Excision of the mobile os hamulus proprius has restored control and sensation of his left hand and enabled him to resume his career as a professional golfer.
Ulnar nerve compression in the hand could be due to a multitude of factors, including a tumour, a ganglion cyst, a fracture of either the pisiform or the hamate, compression in Guyon’s Canal, and an aneurysm of the ulnar artery. [18] To discriminate between a congenital bipartite hamulus or a non union of the hook of the hamate five criteria [17] have been described:
Treatment
There are a limited number of options to treat a mobile hamulus segment causing ulnar nerve compression. [8] Initial splinting of the hand can be trialed to prevent dynamic compression of the nerve in the hope that pain and weakness resolve. [5] Furthermore, avoidance of sports relying on grip strength may provide symptomatic relief. If these interventions do not result in the resolution of symptoms, then there is the option of surgically excising the accessory ossification center on the tip of the hook of the hamate with subsequent decompression and release of the ulnar nerve such as presented in this case.
Consent declaration
Informed consent was obtained from the patient for publication of this case report and accompanying figures. IMAGE ONE is taken from http://upload.wikimedia.org/wikipedia/commons/3/31/Gray422.png. This image is in the public domain because its copyright has expired. This applies worldwide.
Acknowledgments
This paper was written under the supervision of Jeff Ecker from the Western Orthopaedic Clinic in Perth, WA.
Conflict of interest
None declared.
Correspondence
S Moniz: monizsheldon@gmail.com
References
[1] Andress M, Peckar V. Fracture of the hook of the hamate. British Journal of Radiology. 1970;43(506):141-143.
[2] Blum AG, Zabel J-P, Kohlmann R, Batch T, Barbara K, Zhu X, et al. Pathologic Conditions of the Hypothenar Eminence: Evaluation with Multidetector CT and MR Imaging1. Radiographics. 2006;26(4):1021-1044.
[3] Bianchi S, Abdelwahab I, Federici E. Unilateral os hamuli proprium simulating a fracture of the hook of the hamate: a case report. Bulletin of the Hospital for Joint Diseases Orthopaedic Institute. 1990;50(2):205.
[4] Grave K, Brown T. Skeletal ossification and the adolescent growth spurt. American journal of orthodontics. 1976;69(6):611-619.
[5] Chow JC, Weiss MA, Gu Y. Anatomic variations of the hook of hamate and the relationship to carpal tunnel syndrome. The Journal of hand surgery. 2005;30(6):1242-1247.
[6] Greene M, Hadied A. Bipartite hamulus with ulnar tunnel syndrome–case report and literature review. The Journal of hand surgery. 1981;6(6):605.
[7] O’Driscoll SW, Horii E, Carmichael SW, Morrey BF. The cubital tunnel and ulnar neuropathy. Journal of Bone & Joint Surgery, British Volume. 1991;73(4):613-617.
[8] Pierre-Jerome C, Roug I. MRI of bilateral bipartite hamulus: a case report. Surgical and Radiologic Anatomy. 1998;20(4):299-302.
[9] Garzón-Alvarado D, García-Aznar J, Doblaré M. Appearance and location of secondary ossification centres may be explained by a reaction–diffusion mechanism. Computers in biology and medicine. 2009;39(6):554-561.
[10] Freyschmidt J, Brossmann J. Koehler/Zimmer’s Borderlands of Normal and Early Pathological Findings in Skeletal Radiography. TIS; 2003.
[11] Koskinen SK, Mattila KT, Alanen AM, Aro HT. Stress fracture of the ulnar diaphysis in a recreational golfer. Clinical Journal of Sport Medicine. 1997;7(1):63.
[12] Torisu T. Fracture of the hook of the hamate by a golfswing. Clinical orthopaedics and related research. 1972;83:91-94.
[13] Viegas SF, Patterson RM, Hokanson JA, Davis J. Wrist anatomy: incidence, distribution, and correlation of anatomic variations, tears, and arthrosis. The Journal of hand surgery. 1993;18(3):463-475.
[14] Berger R, Garcia-Elias M. General anatomy of the wrist. In: Biomechanics of the wrist joint: Springer; 1991.
[15] SHEA JD, McCLAIN EJ. Ulnar-nerve compression syndromes at and below the wrist. The Journal of Bone & Joint Surgery. 1969;51(6):1095-1103.
[16] LaStayo P, Michlovitz S, Lee M. Wrist and hand. Physical Therapies in Sport and Exercise. 2007:338.
[17] Evans MW, Gilbert ML, Norton S. Case report of right hamate hook fracture in a patient with previous fracture history of left hamate hook: is it hamate bipartite? Chiropractic & osteopathy. 2006;14(1):1-7.
[18] Zeiss J, Jakab E, Khimji T, Imbriglia J. The ulnar tunnel at the wrist (Guyon’s canal): normal MR anatomy and variants. AJR. American journal of roentgenology. 1992;158(5):1081-1085.
