Evaluating women’s knowledge of the combined oral contraceptive pill in an Australian rural general practice setting
Dr Sharna Kulhavy, Dr Teresa Treweek
Tuesday, September 20th, 2016
Background: In addition to the contraceptive action of the combined oral contraceptive pill (COCP), there are a number of other benefits to its use such as menstrual cycle regulation. However, COCP use is also associated with a higher risk of thromboembolism. Despite the prevalence of COCP use, studies have indicated that overall women have poor knowledge of the COCP. Aim: To evaluate women’s knowledge of the COCP in a rural general practice setting. The extent of knowledge was assessed in several domains including: COCP use and effectiveness, mechanism of action, and the risks and benefits of COCP use. Methods: An observational study design was utilised. Women aged 18-50 years self-selected to complete an anonymous survey at a general practice in rural NSW. Women who were currently using, had previously used, or had never used the COCP were invited to participate. Women using a progesterone-only contraceptive were excluded. A total knowledge score on the usage and effects of the COCP was calculated for each participant by assessing responses to 34 questions for an overall score out of 34. Results: A total of 80 surveys were completed revealing that 98% of respondents used the COCP at some time in their lives with almost 29% being current users. The mean total knowledge score for all participants was 14.4 (SD = 4.9) out of a possible 34 (range: 5 – 26). There was no significant difference in total knowledge score between current and previous users (p = 0.56). Conclusion: The women surveyed in this study appear to have substantial gaps in their knowledge of the COCP. This study provides insight into specific knowledge areas that require further education and clarification during COCP counselling sessions (especially those conducted by a GP) to encourage improved knowledge of the COCP by women in this particular setting.
Introduction
The combined oral contraceptive pill (COCP) is an oral hormonal contraceptive that contains synthetic oestrogen and progesterone. Since it was first made available in Australia in 1961, the COCP has become the principal contraceptive method of choice among Australian women [1]. Contraceptive management is a common reason for GP consultation, with the COCP being the most frequently prescribed contraceptive [1].
Though it is well known for its contraceptive action, there are a number of additional benefits associated with COCP use [2-11]. There is decreased risk of ovarian and endometrial cancers [2,3,5,6] and reduced risk of benign breast disease, functional ovarian cysts, ectopic pregnancies, and pelvic inflammatory disease [2-4,7]. The COCP is also beneficial in that it helps to regulate the menstrual cycle, and reduces dysmenorrhoea, menorrhagia, and endometriosis-associated pain [2,3,8,9]. Acne and the effects of hyperandrogenism may also be minimised with COCP use [2-4,10].
Despite these many benefits, there are several risks associated with COCP use. The introduction of low-dose COCPs saw a significant improvement in its safety profile, particularly in the reduction of thromboembolism [2,3]. Nonetheless, COCP use does increase the risk of thromboembolism, stroke, and myocardial infarction [2,3,12,13]. This is a rare complication in otherwise healthy women [2]. Women over the age of 35, smokers, and women who are obese have a higher risk of thromboembolism with COCP use [11,14]. The evidence is mixed as to whether the COCP increases the risk of breast cancer [2,15]. The current consensus is that the COCP does increase risk, but this risk is considered to be very small (equal to approximately one extra case per year for every 100,000 women) and becomes negligible ten years after cessation of use [15,16], however, research is still ongoing.
The COCP has been shown to be a very effective contraceptive with perfect use (the failure rate is 0.3%), however, its typical-use failure rate is as high as 9% [17,18]. These figures were generated by an American study by Trussell [18] and are frequently utilised in Australian literature. The typical-use rate is most commonly attributed to incorrect or inconsistent use [2]. Thus, unplanned pregnancy is an important risk for women taking the COCP to consider. There is little data to suggest that sound knowledge of the COCP correlates to improved behavioural changes and related outcomes such as unintended pregnancies [19,20]. Nevertheless, a better understanding of this common medication is likely to be a significant contributing factor in the reduction of the current failure rate which is why studies assessing women’s knowledge of the COCP are important.
Research conducted in a diverse range of settings has indicated that women’s knowledge of the COCP is generally poor [11,19,21-24]. A comprehensive search of the current literature, however, revealed a paucity of studies focusing on such knowledge amongst rural Australian women, with only one Australian study focusing on women’s knowledge of the COCP from a national perspective [11]. Furthermore, there were no international studies focusing on a rural perspective in their study populations. As such, this study aimed to evaluate the level of knowledge women attending an Australian rural general practice have regarding the COCP. The extent of knowledge was assessed through several domains including: COCP use and effectiveness, mechanism of action, and the potential risks and benefits of COCP use.
Methods
Participants
Participants eligible for inclusion were women of reproductive age, between 18 and 50 years, who were patients of a New South Wales rural general practice, and who attended the practice during the study period. Women who were currently using or had previously used the COCP were invited to participate, as were women who had never taken the COCP. Male patients and women taking a progesterone-only oral contraceptive were excluded from this study due to the nature of the research question. A total of 80 responses were collected and all were used in data analysis.
Study design and survey
This study utilised an observational study design through the provision of a survey to participants. The survey included two basic demographic questions (age and level of education) and five questions assessing personal COCP usage patterns. The questions assessing knowledge covered several domains including: COCP use and effectiveness, mechanism of action, and the potential risks and benefits of COCP use. Additionally, participants were asked about their information sources regarding the COCP.
Recruitment and data collection
Women attending the medical practice self-selected to complete the survey. Participant information sheets were attached to each survey and were made available at the reception desk of the practice. Posters advertising the survey were also displayed in the waiting room area. Participation was entirely voluntary and anonymous, with consent being implied from completion of the survey. Completed surveys were returned to a secure box at the reception desk, with access to returned surveys and subsequent generated data being limited exclusively to the lead researcher. Data collection occurred between October and December 2014.
Ethics approval was granted by the University of Wollongong (UoW) Human Research Ethics Committee in collaboration with the UoW Graduate School of Medicine.
Statistical analysis
Survey data was processed using Microsoft Excel™. P-values were calculated for correct scores between current and previous COCP users using z-scores with a significance level of ≤ 0.05.
A “total knowledge score” was also calculated for each participant by combining the total marks for questions 8, 10, and 11 of the survey, where one mark was awarded to each correct response. Question 8 comprised a total of 6 sub-questions, question 10 comprised 13 and question 11 had 15. As such, the maximum possible score for these questions was 34. The mean total knowledge score was subsequently calculated by averaging the values amongst all the participants. The total knowledge scores of current COCP users versus previous users were analysed using the Mann-Whitney “U test” with a significance level of ≤ 0.05.
For the purpose of this study, a score of 80% or above for each individual response item was designated as an adequate level of knowledge.
Results
Sample characteristics
In total, 80 responses were received during the study period. Table 1 shows basic demographic information of the study participants. The mean age of the sample was 32.1 years (standard deviation = 8.8).
Table 1: Demographic information of sample (n = 80)
| Variable | n (%) |
| Q.1 Age (years) | |
| 18-20 | 8 (10%) |
| 21-24 | 17 (21%) |
| 25-30 | 10 (13%) |
| 31-34 | 17 (21%) |
| 35-40 | 11 (14%) |
| 40-50 | 17 (21%) |
| Q.2 Education level | |
| Year 10 | 18 (23%) |
| Year 12 | 24 (30%) |
| Undergraduate degree | 16 (20%) |
| Postgraduate degree | 6 (8%) |
| TAFE qualification | 12 (15%) |
| Other | 4 (5%) |
Personal COCP usage information
Of the respondents, 98% (n = 78) had taken the COCP at some point in their lives (question 3 of the survey). Further information regarding usage for women who had previously or were currently taking the COCP is listed in Table 2. Women who had never taken the COCP were not required to complete these questions (questions 4 to 7).
Table 2: Usage information for women who are currently using or have previously used the COCP
| Variable | n (%*) |
| Q.4 Current COCP usage (n = 78) | |
| Yes | 23 (29%) |
| No | 55 (69%) |
| Q.5 Duration of COCP usage (n = 77) | |
| < 1 year | 5 (6%) |
| 1 – 5 years | 29 (36%) |
| 5 – 10 years | 17 (21%) |
| > 10 years | 26 (33%) |
| Q.6 Has an active tablet ever been missed? (n = 78) | |
| Yes | 64 (80%) |
| No | 13 (16%) |
| Don’t Know | 1 (1%) |
| Q.7 Frequency of missing an active tablet (n = 77) | |
| Never | 12 (15%) |
| Only one time | 4 (5%) |
| Once a year | 11 (14%) |
| Once every few months | 30 (38%) |
| Once a month | 16 (20%) |
| Once a week | 4 (5%) |
*Percentages calculated using the total sample (n = 80)
Knowledge domains
COCP use and effectiveness
Participants were asked to complete questions that assessed their general knowledge of the COCP and of what factors may reduce the COCPs contraceptive effect.
In terms of general knowledge (question 8 of the survey), 96% of participants correctly identified that the COCP needs to be taken every day to serve as effective contraceptive, with 94% correctly identifying that it should be taken at the same time every day. Only 28% of women were aware that the COCP is not the most effective contraceptive currently available with 13% of current COCP users selecting the correct answer (compared to 35% of previous users).
Of the factors that may reduce the contraceptive effect of the COCP (question 10), missing one active pill by more than 12 hours and missing more than one active pill was correctly identified by 84% and 94% of women respectively. Other factors that potentially reduce contraceptive effect (with percentage of participants selecting the correct response in brackets) are as follows: St John’s wort (20%), epilepsy medications (14%), vomiting (79%), and severe diarrhoea (61%). Two-thirds of women incorrectly identified that antibiotics (other than rifampicin and rifabutin) may be a factor that reduces contraceptive benefit. There was no significant difference in the number of participants selecting the correct response between current and previous COCP users for each of the factors investigated. Participant responses are further detailed in Table 3.
Table 3: Participant responses to general knowledge questions relating to the COCP and factors that may reduce its contraceptive action
| Yes | No | Don’t know | No response | Number of current COCP users correct (n = 23) | Number of previous COCP users correct
(n = 55) |
P-value
(significance ≤ 0.05) |
|
| Q.8 General knowledge | |||||||
| The pill needs to be taken every day to be an effective contraceptive | *77 (96%) | 1 (1%) | – | 2 (3%) | 22 (96%) | 53 (96%) | 0.88 |
| The pill should be taken at approximately the same time every day | *75 (94%) | 3 (4%) | 2 (3%) | – | 23 (100%) | 51 (93%) | 0.18 |
| It is acceptable to continue taking active tablets without taking the inactive tablets in between | *43 (54%) | 16 (20%) | 21 (26%) | – | 12 (52%) | 31 (56%) | 0.73 |
| The pill is the most effective form of contraception currently available when used correctly | 44 (55%) | *22 (28%) | 14 (18%) | – | 3 (13%) | 19 (35%) | 0.054 |
| It is possible to fall pregnant while taking the pill even with perfect use | *63 (79%) | 10 (13%) | 6 (8%) | 1 (1%) | 16 (70%) | 45 (82%) | 0.23 |
| It is important to take a break from using the pill | 26 (33%) | *20 (25%) | 34 (43%) | – | 6 (26%) | 14 (25%) | 0.95 |
| Q.10 Factors that may reduce the contraceptive benefit of the COCP | |||||||
| Missing one active pill by less than 12 hours | 25 (31%) | *34 (43%) | 17 (21%) | 4 (5%) | 11 (48%) | 23 (42%) | 0.62 |
| Missing one active pill by more than 12 hours | *67 (84%) | 6 (8%) | 7 (9%) | – | 19 (83%) | 48 (87%) | 0.58 |
| Missing more than one active pill | *75 (94%) | 1 (1%) | 3 (4%) | 1 (1%) | 23 (100%) | 51 (93%) | 0.18 |
| Missing one or more inactive pill/s | 22 (28%) | *43 (54%) | 14 (18%) | 1 (1%) | 14 (61%) | 28 (51%) | 0.42 |
| St John’s Wort herbal preparation | *16 (20%) | 9 (11%) | 55 (69%) | – | 5 (22%) | 11 (20%) | 0.86 |
| Epilepsy medications such as phenytoin or carbamazepine | *11 (14%) | 3 (4%) | 66 (83%) | – | 3 (13%) | 8 (15%) | 0.86 |
| Vomiting | *63 (79%) | 5 (6%) | 12 (15%) | – | 19 (83%) | 44 (80%) | 0.79 |
| Severe diarrhoea | *49 (61%) | 10 (13%) | 21 (27%) | – | 15 (65%) | 34 (62%) | 0.78 |
| Smoking | 6 (8%) | *36 (45%) | 38 (48%) | – | 9 (39%) | 26 (47%) | 0.51 |
| Antibiotics such as rifampicin and rifabutin | *53 (66%) | 3 (4%) | 24 (30%) | – | 14 (61%) | 38 (69%) | 0.48 |
| Other antibiotics
(When taken without side-effects like vomiting/diarrhoea) |
53 (66%) | *2 (3%) | 25 (31%) | – | 0 (0%) | 2 (4%) | 0.35 |
| Minor alcohol consumption
(e.g. an occasional alcoholic drink/s not on a regular basis) |
6 (8%) | *52 (65%) | 22 (28%) | – | 17 (74%) | 35 (64%) | 0.38 |
| Excessive alcohol consumption
(e.g. drinking amounts that cause vomiting, diarrhoea, poor concentration or memory, or significant liver damage) |
*43 (54%) | 13 (16%) | 24 (30%) | – | 10 (43%) | 32 (58%) | 0.23 |
*Indicates the correct answer
Mechanism of action
Only 58% of women surveyed correctly identified that the COCP acts to prevent ovulation; this represented 44% of current COCP users and 64% of previous COCP users. Furthermore, only 3% of the study sample correctly identified all three mechanisms of action (preventing ovulation, thickening of cervical mucus, and helping to prevent adherence of the embryo to the endometrium).
Risks and benefit of COCP use
Frequencies of responses to questions assessing knowledge of the potential risks and benefits of the COCP are shown in Table 4. The conditions in which COCP use may be beneficial (with the percentages of participants selecting the correct responses listed in brackets) were as follows: menstrual disturbances (60%), acne (56%), endometriosis-associated pain (28%), ectopic pregnancy (9%), and ovarian and endometrial cancer (6%). Fifty-nine percent of women correctly identified that the COCP has no effect on the risk of contracting a sexually transmitted infection (STI). Furthermore, weight gain was incorrectly identified as a risk associated with taking the COCP by 75% of women with only 5% of participants selecting the correct answer of “no effect”. COCP use increases the risk of cardiovascular disease which 39% of women correctly identified. For the majority of these questions, “don’t know” was the response selected by a large proportion of participants.
Table 4: Participant responses regarding effects of the COCP on level of risk for various conditions
| Q.11 | Decreases | No effect | Increases | Don’t know | No response | Number of current COCP users correct (n=23) | Number of previous COCP users correct
(n=55) |
P-value
(significance ≤ 0.05) |
| Ectopic pregnancy | *7 (9%) | 18 (23%) | 11 (14%) | 44 (55%) | – | 2 (9%) | 4 (7%) | 0.83 |
| Birth defects | 2 (3%) | *33 (41%) | 8 (10%) | 37 (46%) | – | 4 (17%) | 29 (53%) | 0.004 |
| Infertility | 3 (4%) | *30 (38%) | 14 (18%) | 33 (41%) | – | 9 (39%) | 21 (38%) | 0.94 |
| Cardiovascular disease
(stroke, hypertension, clots) |
2 (3%) | 14 (18%) | *31 (39%) | 33 (41%) | – | 10 (43%) | 21 (38%) | 0.66 |
| Benign breast disease | *4 (5%) | 17 (21%) | 16 (20%) | 42 (53%) | 1 (1%) | 0 (0%) | 4 (7%) | 0.18 |
| Functional ovarian cysts | *9 (11%) | 12 (15%) | 11 (14%) | 47 (59%) | 1 (1%) | 4 (17%) | 5 (9%) | 0.29 |
| Endometriosis-associated pain | *22 (28%) | 9 (11%) | 3 (4%) | 45 (56%) | 1 (1%) | 8 (35%) | 14 (25%) | 0.41 |
| Breast cancer | 4 (5%) | 17 (21%) | *18 (23%) | 41 (51%) | – | 6 (26%) | 13 (22%) | 0.82 |
| Ovarian cancer | *5 (6%) | 18 (23%) | 11 (14%) | 46 (58%) | – | 2 (9%) | 3 (5%) | 0.59 |
| Endometrial cancer | *5 (6%) | 18 (23%) | 7 (9%) | 50 (63%) | – | 1 (4%) | 4 (7%) | 0.63 |
| Menstrual disturbances | *48 (60%) | 6 (8%) | 9 (11%) | 13 (16%) | 4 (5%) | 12 (52%) | 35 (64%) | 0.35 |
| Acne | *45 (56%) | 4 (5%) | 14 (18%) | 16 (20%) | 1 (1%) | 11 (48%) | 33 (60%) | 0.32 |
| Weight gain | 1 (1%) | *4 (5%) | 60 (75%) | 13 (16%) | 2 (3%) | 1 (4%) | 3 (5%) | 0.84 |
| Pelvic inflammatory disease | *6 (8%) | 14 (18%) | 9 (11%) | 50
(63%) |
1 (1%) | 2 (9%) | 4 (7%) | 0.83 |
| Sexually transmitted infections | 4 (5%) | *47 (59%) | 7 (9%) | 20 (25%) | 2 (3%) | 11 (48%) | 36 (65%) | 0.12 |
*Indicates the correct answer
Question 12 of the survey asked women to identify factors that can potentially increase a women’s risk of thromboembolism while taking the COCP. The most frequently identified risk factors were smoking and obesity (selected by 74% and 69% of participants, respectively). Only 38% correctly identified all three risk factors, which also includes age greater than 35 years [11,14].
Information sources
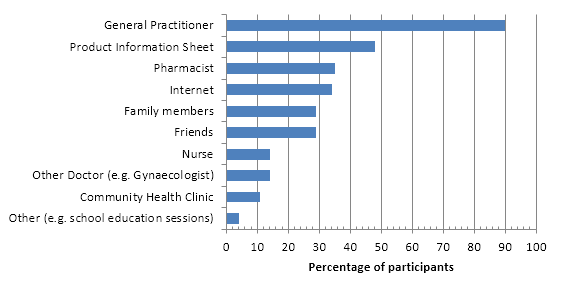
Participants were asked where they source information regarding the COCP for question 13 of the survey. “General practitioner” was the most frequently selected option at 90% (n = 72). Further response details are shown in Figure 1.
Figure 1: Survey participants’ information sources regarding the COCP
Total knowledge score
The mean total knowledge score for all participants was 14.4 (SD = 4.86) out of a possible 34 (range = 5 to 26). The mean total knowledge score for current COCP users was 14.0 (SD = 4.81), with previous COCP users achieving a mean score of 14.8 (SD = 4.75). Women who had never used the COCP achieved a mean total knowledge score of 6.5. There was no significant difference in total knowledge score between current and previous users of the COCP (p = 0.56).
Discussion
This study has found deficiencies in women’s knowledge of the COCP in all domains that were assessed. This finding is consistent with the available literature [11,19,21-24]. For the purpose of this study, a score of 80% or above for each individual response item was designated as an adequate level of knowledge. The rationale for stating an arbitrary value such as this was influenced by a recent systematic review by Hall et al. [19]. Though many studies concluded women have a poor level of knowledge regarding oral contraceptives, Hall et al. stated that of the studies they included for review, “what constituted deficient or adequate knowledge was not clearly defined”. The majority of women did not score above the required 80% correct responses to be considered adequate knowledge. No significant differences were found in the number of correct responses per question between current COCP users and previous users except for one question regarding whether the COCP has an effect on the risk of birth defects occurring (p = 0.004). Furthermore, the total knowledge score for both current and previous COCP users was less than 50% of the possible maximum score.
Several key findings discussed below stand out as being important focus areas for improved contraceptive counselling.
COCP use and effectiveness
This study revealed that 55% of women believe the COCP is the most effective form of contraception currently available when used correctly, with only 13% of current COCP users correctly identifying that it is not. Examples of contraception that have a better failure rate profile than the COCP include long-acting reversible contraceptives (LARC) such as the implantable rod (typical and perfect-use failure rate 0.05%), and intrauterine devices such as the Mirena (typical and perfect-use failure rate 0.2%) [17].
Women were not aware that antibiotics (other than rifampicin and rifabutin) were no longer considered to have a negative impact on the contraceptive effect of the COCP [25], with 66% of women indicating that taking antibiotics (without side effects such as vomiting and diarrhoea) would reduce the contraceptive effect of the COCP.
There were mixed results regarding whether it is important to take a break from the COCP with 25% of women correctly identifying there is no requirement for a break. Interestingly, Philipson, Wakefield, and Kasparian [11] found that 25.6% of their participants thought that it was healthy to stop COCP use for a while (length of time was not stipulated in the question).
Mechanism of action
Only 58% of women correctly identified the main mechanism by which the COCP works, with 3% correctly identifying all three mechanisms. A systematic review by Hall et al. [19] found that understanding of the mechanism of action is infrequently assessed in similar studies. A study by Rajasekar and Bigrigg [23] not included in the aforementioned review found that 81.5% of women understood that the oral contraceptive prevented ovulation every month, but that 32% also thought that it killed sperm.
Risks of COCP use
Of the study participants, 39% correctly identified that the COCP increases the risk for cardiovascular disease (hypertension, stroke, and other thromboembolic events). Similarly, Philipson, Wakefield, and Kasparian [11] found that 46.5% women identified an increase in blood clots. Although 74% of women in our study identified smoking as a factor that when combined with the COCP increases thromboembolism risk further, only 38% of women correctly identified all three risk factors (obesity, age over 35 years, and smoking).
Women appear to erroneously believe that the COCP causes weight gain (75% of respondents). A causal relationship has never been established. A Cochrane Review has found there is no significant difference in weight change between placebo and those taking combined contraceptives, though further research was indicated [26]. Previous studies suggest similar results. Fletcher, Bryden, and Bonin [27] found that 30.6% of respondents were concerned about weight gain on the pill, with 23.4% of respondents reporting weight gain as an experienced side effect. Gaudet et al. [28] found that 51.5% of respondents thought weight would increase on the pill.
Only 59% of women were aware that the COCP has no effect on contracting STIs, with 48% of current COCP users identifying the correct answer. This result is lower than that found by Philipson, Wakefield, and Kasparian [11] with 81.3% of their respondents identifying the correct answer.
Benefits of COCP use
There was a low level of understanding regarding decreased ovarian and endometrial cancer risk, but a better (though still low) understanding that COCP use can improve acne and menstrual disturbances. Poor understanding about COCP benefits appears consistent among studies with Philipson, Wakefield, and Kasparian [11] finding 13.7% correctly identified that COCP use decreases ovarian cancer risk, with 10% identifying decreased risk of endometrial cancer.
Study limitations
Noting that approximately 29% of this study sample is currently taking the COCP, one might consider that knowledge would be forgotten after having ceased the COCP or after changing contraceptive methods. Additionally, it cannot be expected that women will remember all details relating to the COCP, as with any medication. Significant limitations of this study include the small response rate, which is likely due to the self-selection of participants. A self-selection bias may also exist. We can see from the results that there were very few women who had never taken the pill completing the survey. We must consider whether this is a true representation, or whether this may reflect the fact that women who have previously taken or are currently taking the COCP are more likely to complete the survey (perhaps due to a perceived familiarity with the topic). As the study was conducted in a general practice, a bias may also exist towards women who are likely to attend such medical facilities. An additional limitation of this study is that data was generated out of a single general practice and therefore the results may reflect specific factors associated with the GPs working there. Due to how the study was implemented, it cannot be determined if the participants had ever received contraceptive counselling from the practitioners within this centre, or whether a single or multiple GPs from this practice may have been involved in the counselling and prescribing of the COCP. At the time the study was conducted, seven GPs were working within the practice and so participants are likely patients of a number of these GPs with no particular focus on an individual practitioner’s patient list. Both the self-selection and single-centre nature of this study means that the results cannot be generalised. The survey was developed after a review of current literature and did not come from a validated source. Assessment of the reading level of the survey and a pilot study prior to data collection would improve the validity of the findings. Additionally, statistical analysis was limited to current and previous COCP users as the sample of participants who had never used the COCP was too small to allow reliable calculations.
Implication for clinical practice and future directions
A recent analysis of the Bettering the Evaluation and Care of Health (BEACH) data by Mazza et al. [1] found that COCP prescribing is a common focus of many GP consultations concerning contraceptive management. Our study also indicated that GPs are the main source of information regarding the COCP. Given that the COCP is a prescription medication, routine medical consultations are required and offer ample opportunity for medical practitioners to ensure appropriate use and knowledge of the COCP. This is especially so since a total of 54% of participants in our study indicated they have been or were using the pill for more than five years. In their study assessing Australian women’s knowledge of the COCP, Philipson, Wakefield, and Kasparian [11] found a positive correlation between duration of pill usage and level of knowledge.
Although our study suggested that GPs are the main source of information regarding the COCP, there were many other information sources identified and so we cannot assume the subsequent level of knowledge of the surveyed participants is the result of GP intervention alone. Therefore, other healthcare professionals that may provide COCP counselling have a role in helping to improve women’s knowledge of the COCP. Given that the Internet, friends, and family members were also important information sources for women regarding the COCP, awareness and appropriate counselling is also necessary to identify and address any misinformation that women may have obtained from these sources.
This study provides a unique perspective in that it assesses rural Australian women’s knowledge of the COCP. The aforementioned study by Philipson, Wakefield, and Kasparian [11], whose data collection was generated randomly from each state, was the only other Australian study identified after examination of the literature. As our study was limited to a rural general practice setting, future research may wish to expand on this data by investigating other rural practices or compare results to metropolitan practices.
Rural Australians experience poorer health outcomes compared to their metropolitan counterparts [29,30]. Health literacy is likely a contributing factor to such outcomes [30]. An analysis of the Adult Literacy and Life Skills Survey data from 2006 by the Australian Bureau of Statistics shows that health literacy levels are low across the board – 42% of Australian urban populations were shown to have a literacy level of 3 (considered an adequate level) or greater; 38% and 39% of inner regional and remote populations, respectively also demonstrated a literacy level of 3 or greater. The outer regional populations possessed the lowest levels of people demonstrating a literacy level of 3 or greater at 36% [31]. In the context of the clinical environment, there is a paucity of literature available, but one recent study by Wong et al. [32] comparing health literacy of patients attending both a rural and an urban rheumatology practice found no significant difference between these groups. Despite research showing differences in health outcomes between rural and metropolitan populations of Australia [29,30], studies comparing the knowledge and health literacy of rural and metropolitan patients, particularly in relation to medications, proved difficult to find so we cannot extrapolate the findings of the current study to comment on whether a general knowledge deficit exists.
Since this study was designed only to assess women’s level of knowledge about the COCP, and not factors associated with level of knowledge, further studies regarding what factors influence knowledge are also important. These may include factors relating to the primary care setting, such as: impact of consultation timing; exploring the discussions and resources used during COCP consultations and whether counselling deficiencies exist; assessing what information healthcare professionals deem clinically relevant or applicable on an individual patient basis, and whether this impacts upon what information is provided to patients and therefore what knowledge base they retain. Additional studies may wish to investigate the effectiveness of the product information sheet for the COCP, or whether women believe COCP information is easily accessible and where this can be obtained (for example, what limits women’s access to information from pharmacies or community health clinics). Future studies may also wish to explore whether rural specific issues (for example, more limited access to healthcare providers) play a role.
Furthermore, additional studies that evaluate practical strategies for improving knowledge and information retention should also be undertaken. In the systematic review by Hall et al. [19] only four studies assessed interventions and their impact on contraceptive pill knowledge. Three of the four studies noted improved knowledge in at least one domain, highlighting that an array of additional educational materials may be beneficial in improving counselling sessions [19].
As more Australian-specific data accumulates about women’s knowledge of the COCP, better public health initiatives and education strategies can be implemented to improve outcomes. The results of this study may encourage healthcare professionals to better understand and review areas of their own counselling sessions. Improvements may be achieved through better addressing how to use the COCP, what will affect its contraceptive benefit, and common misconceptions. Additionally, healthcare professionals can be assured they have provided appropriate informed consent by discussing risks, benefits, and alternative options [33]. In the long term, this may eventually lead to improvements in the typical failure rate of the COCP and reduce the rate of unintended pregnancies.
Conclusion
The women surveyed in this study appear to have substantial gaps in their knowledge of the COCP despite a high prevalence and duration of usage. Although many other sources were also utilised for information on the COCP, GPs were the main source of information. As such, this study provides insight into specific knowledge areas that require further education and clarification during COCP counselling sessions to encourage improved knowledge of the COCP by women, particularly those in the rural Australian general practice setting.
Acknowledgements
The authors would like to thank the staff at the medical centre where this research was conducted for their support in facilitating this project.
Conflicts of interest
None declared.
References
[1] Mazza D, Harrison C, Taft A, Brijnath B, Britt H, Hussainy S, et al. Current contraceptive management in Australian general practice: an analysis of BEACH data. Med J Aust. 2012;197(2):110-4.
[2] Dragoman M. The combined oral contraceptive pill – recent developments, risks and benefits. Best Pract Res Clin Obstet Gynaecol. 2014;28(6):825-34.
[3] D’Souza R, Guillebaud J. Risks and benefits of oral contraceptive pills. Best Pract Res Clin Obstet Gynaecol. 2002;16(2):133-54.
[4] Schindler A. Non-contraceptive benefits of oral hormonal contraceptives. Int J Endocrinol Metab. 2013;11(1):41-7.
[5] Collaborative group on epidemiological studies on endometrial cancer. Endometrial cancer and oral contraceptives: an individual participant meta-analysis of 276 women with endometrial cancer from 36 epidemiological studies. The Lancet Oncology. 2015; 16(9):1061-70.
[6] Havrilesky L, Moorman P, Lowery W, Gierisch J, Coeytaux R, Myers E, et al. Oral contraceptive pills as primary prevention for ovarian cancer. J. Obstet Gynecol. 2013;122(1):139-47.
[7] Vessey M, Yeates D. Oral contraceptives and benign breast disease: an update of findings in a large cohort study. Contraception. 2007; 76(6): 418-24.
[8] Harada T, Momoeda M, Taketani Y, Hoshiai H, Terakawa N. Low-dose oral contraceptive pill for dysmenorrhea associated with endometriosis: a placebo-controlled, double-blind, randomized trial. Fertility and Sterility. 2008;90(5)1583-8.
[9] Wong C, Farquhar C, Roberts H, Proctor M. Oral contraceptive pill for primary dysmenorrhoea. Cochrane Database Syst Rev. 2009.
[10] Arowojolu A, Gallo M, Lopez L, Grimes D. Combined oral contraceptive pills for treatment of acne. Cochrane Database Syst Rev. 2012.
[11] Philipson S, Wakefield C, Kasparian N. Women’s knowledge, beliefs, and information needs in relation to the risks and benefits associated with use of the oral contraceptive pill. Int. J. Wom. Health. 2011;20(4):635-42.
[12] de Bastos M, Stegeman B, Rosendaal F, Van Hylckama Vlieg A, Helmerhorst F, Stijnen T, et al. Combined oral contraceptives: venous thrombosis. Cochrane Database Syst Rev. 2014.
[13] Roach R, Helmerhorst F, Lijfering W, Stijnen T, Algra A, Dekkers O. Combined oral contraceptives: the risk of myocardial infarction and ischemic stroke. Cochrane Database Syst Rev. 2015.
[14] Royal College of Obstetricians and Gynaecologists (RCOG). Green-top guideline No.40: Venous thromboembolism and hormonal contraception [Internet]. RCOG; 2010 [cited 2015 March 24]. Available from: https://www.rcog.org.uk/en/guidelines-research-services/guidelines/gtg40/.
[15] Royal Australian and New Zealand College of Obstetricians and Gynaecologists (RANZCOG). College Statement C-Gyn 28: Combined hormonal contraceptives [Internet]. RANZCOG; 2012 [cited 2015 March 24]. Available from: https://www.ranzcog.edu.au/college-statements-guidelines.html#gynaecology.
[16] Cancer Council Australia. Position Statement: Combined oral contraceptives and cancer risk [Internet]. Cancer Council Australia; 2006 [cited 2015 Feb 7]. Available from: http://www.cancer.org.au/policy-and-advocacy/position-statements/oral-contraceptives.html.
[17] eTG Complete [Internet]. Melbourne (Vic): Therapeutic Guidelines Limited; 2015. Hormonal contraception: introduction; [cited 2015 March 24]. Available from: http://online.tg.org.au.ezproxy.uow.edu.au/ip/desktop/index.htm.
[18] Trussell J. Contraceptive failure in the United States. Contraception. 2011;83(5):397-404.
[19] Hall K, Castaño P, Stone P, Westhoff C. Measuring oral contraceptive knowledge: a review of research findings and limitations. Patient Educ Couns. 2010;81(3):388-94.
[20] Black K, Bateson D, Harvey C. Australian women need increased access to long-acting reversible contraception. Med J Aust. 2013;199(5):317-8.
[21] Bryden P, Fletcher P. Knowledge of the risks and benefits associated with oral contraception in a university-aged sample of users and non-users. Contraception. 2001;63(4):223-7.
[22] Davis T, Fredrickson D, Potter L, Brouillette R, Bocchini A, Parker R, et al. Patient understanding and use of oral contraceptive pills in a southern public health family planning clinic. South Med J. 2006;99(7):713-8.
[23] Rajasekar D, Bigrigg A. Pill knowledge amongst oral contraceptive users in family planning clinics in Scotland: facts, myths and fantasies. Eur J Contracept Reprod Health Care. 2000;5(1):85-90.
[24] Schrager S, Hoffmann S. Women’s knowledge of commonly used contraceptive methods. WMJ. 2008;107(7):327-30.
[25] Family Planning New South Wales, Family Planning Queensland, Family Planning Victoria. Contraception: an Australian clinical practice handbook. 3rd ed. Canberra: Family Planning New South Wales, Family Planning Queensland, Family Planning Victoria; 2012.
[26] Gallo M, Lopez L, Grimes D, Carayon F, Schulz K & Helmerhorst F. Combination contraceptives: effects on weight. Cochrane Database Syst Rev. 2014 Jan
[27] Fletcher P, Bryden P, Bonin E. Preliminary examination of oral contraceptive use among university-aged females. Contraception. 2001;63(4):229-233.
[28] Gaudet L, Kives S, Hahn P, Reid R. What women believe about oral contraceptives and the effect of counselling. Contraception. 2004;69(1):31-6.
[29] Australian Institute of Health and Welfare (AIHW). Rural, regional and remote health: Indicators of health status and determinants of health [Internet]. AIHW; 2008 [cited 2016 May 4]. Available from: http://www.aihw.gov.au/publication-detail/?id=6442468076.
[30] Australian Institute of Health and Welfare. Australia’s health 2014 [Internet]. AIHW; 2014 [cited 2016 May 4]. Available from: http://www.aihw.gov.au/WorkArea/DownloadAsset.aspx?id=60129548150.
[31] Australian Bureau of Statistics (ABS). Health literacy Australia 2006 [Internet]. ABS; 2008 [cited 2016 May 4]. Available from: http://www.abs.gov.au/ausstats/abs@.nsf/Latestproducts/4233.0Main%20Features22006?opendocument&tabname=Summary&prodno=4233.0&issue=2006&num=&view=.
[32] Wong P, Christie L, Johnston J, Bowling A, Freeman D, Bagga H, et al. How well do patients understand written instructions? Health literacy assessment in rural and urban rheumatology outpatients. Medicine. 2014;93(25):1-9.
[33] Vogt C, Schaefer M. Disparities in knowledge and interest about benefits and risks of combined oral contraceptives. Eur J Contracept Reprod Health Care. 2011;16(3);183-93.